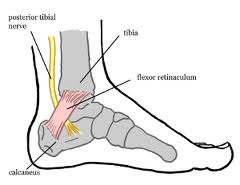
The tarsal tunnel is a narrow tunnel that lies on the inside of the ankle. It allows the posterior tibial artery, vein, tendon and nerve to run through from the leg into the foot. It is also the pathway for the flexor digitorum longus and flexor hallucis longus tendons coming into the foot.
The structures within this tunnel are maintained and protected by a thick ligament band (flexor retinaculum).
Compression of the posterior tibial nerve, as it travels through this tarsal tunnel gives rise to the condition known as Tarsal Tunnel Syndrome (TTS). The posterior tibial nerve passes through the tarsal tunnel and separates into three different branches going into the foot to provide feeling and feedback in the following areas:
- Calcaneal nerve– continues to the heel.
- Medial plantar nerves– continues to the inside sole of the foot.
- Lateral plantar nerves– continues to the outside sole of the foot.
Patients with TTS typically complain of neurological symptoms in the foot, traveling to the big toe and the 3 lesser toes. Sometimes if the pinching of the nerve is higher up in the ankle, it can affect the arch, heel and even calf.
Inflammation or swelling can also occur within the tarsal tunnel for various reasons. This increased fluid can take up room within the tarsal tunnel causing compression on the posterior tibial nerve.
TTS can greatly impact patients’ quality of life if not treated. Depending on the severity, simple tasks such as walking short distances can become almost unbearable.
Causes of Tarsal Tunnel Syndrome (Nerve Damage)
TTS results with compression of the posterior tibial nerve, such as:
- Flat feet– rolling in of the ankle can place compression on the posterior tibial nerve on the inside of the ankle.
- Abnormal tissue growth– within the tarsal tunnel region (varicose vein, benign tumor, ganglion cyst, swollen tendon sheath, and/or arthritic bone spur).
- Physical injury– such as an ankle sprain, or fracture causing inflammation and swelling in or near the tunnel, resulting in compression of the nerve.
- Systemic diseases– such as diabetes or arthritis can cause swelling, and impingement of the nerve.
- Strenuous activities– such as running and jumping.
- Neurofibromatosis- fibrous masses that can form around nerves and have the ability to invade the tarsal tunnel.
- Idiopathic– unknown cause.
Symptoms of Tarsal Tunnel Syndrome (Nerve Damage)
- Neural sensations, such as tingling, burning, pins and needles, hot and cold and/or stabbing pains around the ankles.
- Numbness or pain in the toes, arch, heel, and calf depending on the level of impingement to the nerve.
- Numbness and possible swelling of the foot.
- Cramp sensations, as small muscles within the foot lose their nerve supply.
- Sudden onset of symptoms and often brought on or aggravated by overuse of the foot, prolonged standing and/or beginning a new exercise regime.
- Symptoms when driving, if the foot is in dorsiflexion.
- Positive Tinel’s sign (tapping over the affected nerve on the inside of the ankle will produce a tingling or electric shock sensation over the area and sole of foot).
Diagnosis of Tarsal Tunnel Syndrome (Nerve Damage)
- Patients pain history and a positive Tinel’s sign when you tap over the inside of the ankle.
- Abnormal foot biomechanics, such as flat feet +/- swelling in the foot.
- Palpation around the area to feel if a small mass is present.
- Advance imaging studies (X-ray, Ultrasound or MRI) if there is any suspicion of a mass or initial treatment does improve symptoms.
Treatment for Tarsal Tunnel Syndrome (Nerve Damage)
Should be immediate, to prevent further injury and permanent nerve damage. The symptoms of TTS may mimic other more commonly encountered foot conditions. Therefore it is important to have a proper evaluation by a podiatrist to make the correct diagnosis and get the appropriate treatment.
Non-Surgical Treatment:
- Rest/ Ice/ Nonsteroidal anti-inflammatory drugs – such as ibuprofen, to help reduce pain, inflammation and aid healing.
- Customised foot orthoses- to correct the rolling in of the ankles and reduce compression of the nerve.
- Tibial Nerve Mobilisation/ Foot Mobilisation Therapy– the podiatrist can help mobilise and free the nerve, encouraging normal foot alignment and opening up the ankle joint.
- Injection therapy- local aesthetic to provide pain relief, corticosteroid may be useful in treating the inflammation, prolotherapy to assist with repair of the nerve.
- Supportive footwear– that is professionally fitted, as shoes that are too tight can lead to increased pressure on the tibial nerve.
- Physical therapy- stretching and strengthening exercises of muscles in the legs (tibialis anterior, tibialis posterior, peroneus and flexor digitorum longus).
- Immobilisation (cast/ bracing) – for severe cases immobilising the foot will allow the nerve and surrounding tissue to heal.
- Prescription medication- such as Neurontin, Lyrica and Lidocaine patches for symptom relief.
Surgical Treatment:
If conservative treatment fails, surgery may be necessary to release the nerve within the tarsal tunnel. The incision is made behind the ankle bone, exposing the posterior tibial nerve. This then allows the surgeon to preform the separation of the nerve from the surrounding artery and vein. Soft tissue growth that is causing pressure within the tarsal tunnel is also removed during the procedure.
If scar tissue is evident within the nerve or its branches neurolysis (water technique) is used to remove it. The foot is dressed and non-weight bearing is advised for 1-2 weeks, stitches will be removed around 3 weeks.
Surgery is often the last resort with TTS as some patients experience no improvement or symptoms become worse. Long term management, such as appropriate footwear and customised foot orthoses may be used, as the healing process continues over the next year after surgery.
Related Topics
- Ankle Injury/ Sprains
- Peripheral Neuropathy
- Plantar Fasciitis
- Posterior Tibial Tendon Injury
- Orthotics and Arch Support Therapy
- Foot Mobilisation Therapy
- Prolotherapy